Yoga for Veterans with Back Pain? YES!
 Low back pain (LBP) is one of the most common conditions for which people seek medical care. Unfortunately, for about 20-30% of those who experience LBP, it becomes chronic (lasting more than 12 weeks).
Low back pain (LBP) is one of the most common conditions for which people seek medical care. Unfortunately, for about 20-30% of those who experience LBP, it becomes chronic (lasting more than 12 weeks).
The World Health Organization (WHO) reports that LBP is the “single leading cause of disability worldwide.” On a more positive note, they also report that it is “the condition for which the greatest number of people may benefit from rehabilitation.”
The risk of addiction and overdose deaths associated with opioid pain medications for non-acute conditions, such as LBP, have turned the attention to nonpharmacological treatments over the last few decades. This has provided more research showing the effectiveness of these treatments.
In the US, both active-duty and military veterans have significantly higher rates of chronic pain than their civilian counterparts, with back pain being the most common type.
Researchers recruited 150 veterans who were receiving care at a VA Medical Center in California from 2013-2015 to study how yoga could be used to treat chronic LBP (cLBP). Participants had a diagnosis of cLBP lasting 6 months or longer. They were divided into cohorts and each received a baseline assessment including Roland–Morris Disability Questionnaire (RMDQ) and Brief Pain Inventory (two tools well established to assess back pain and functional limitations), and were instructed to continue their normal care.
The participants were randomized into an experimental group and a delayed treatment group. The experimental group were asked to attend two 60-minute, instructor-led yoga sessions each week. The hatha yoga sessions were designed for people with cLBP who were beginners at yoga and consisted of physical yoga postures, movement sequences, and regulated breathing. These participants were also given brief meditations and a home manual and asked to perform 15-20 minutes of yoga at home on the days they did not attend the instructor-led session. They were asked to record these home sessions including: days home practice occurred, duration of practice, the estimated physical exertion level, and whether an instructor, video, or other guide was used. Participants in the delated treatment group were asked not to participate in yoga until after their 6-month assessment.
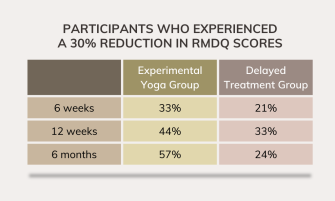
All participants were assessed at baseline, 6 weeks, 12 weeks, and 6 months. After analysis, differences between the two groups were revealed. Both groups experienced reduced scores on the RMDQ at 12 weeks, but the yoga group had a 2.05-point reduction while the other group’s reduction was only 1.29-points. Additionally, at the 6-month assessment, the scores for the yoga group continued to drop, while the other group scores had begun to increase back towards baseline. A 30% reduction in RMDQ score is considered to be a “clinically meaningful outcome”. By the end of the 6 months, over half of the experimental yoga group had met this threshold, while just under a quarter of the delayed treatment group achieved that reduction.
For the secondary outcome, significant differences were observed at all 3 assessments, with larger decreases in pain intensity for the yoga participants.
These findings of hatha yoga having a positive effect on cLBP echo what previous studies had shown in studies involving mostly female civilians. However, there was an increased time for the improvement to be seen in this study. Researchers suggest that VA patients being predominantly male, on average older, and representing a lower attendance rate when compared to the other studies could play a significant role in the delay. However, the fact that the improvement did come, despite these other factors helps to support that yoga can be utilized as an effective tool in helping people, both civilian and military, who are living with cLBP.
Yoga is just one of the many nonpharmacological treatments being proven to be effective as treatments for cLBP as well as many other types of musculoskeletal pain. Your doctor of chiropractic will do a complete exam and history in order to determine a proper course of treatment for your health conditions and your health goals. Suggested lifestyle modifications to help you manage pain could include yoga, other physical activities, and nutritional dietary changes, among other options. The complete treatment plan your chiropractic physician provides will work together to help you reduce pain, improve overall health and maximize function, enabling you to put your focus on people and activities you enjoy.
RESOURCES:
Groessl EJ, Liu L, Chang DG, Wetherell JL, Bormann JE, Atkinson JH, Baxi S, Schmalzl L. Yoga for Military Veterans with Chronic Low Back Pain: A Randomized Clinical Trial. Am J Prev Med. 2017 Nov;53(5):599-608. doi: 10.1016/j.amepre.2017.05.019. Epub 2017 Jul 20. PMID: 28735778; PMCID: PMC6399016.
World Health Organization. Low Back Pain. https://www.who.int/news-room/fact-sheets/detail/low-back-pain 19 June 2023 Accessed Jan 22, 2024.